Date Posted: Monday,
August 12, 2013
By: Yvonne D. Dailey, CPC, CPC-I
This topic was so popular at AAPC's National Conference in Orlando that it made sense to share an overview of the session to anyone who may have missed it. Also, with AAPC's new Certified Professional Biller (CPB) credential, we are sure to see more education on the revenue cycle at upcoming AAPC events, like next year's National Conference in Nashville (April 13-16).
Every practice should be run like a business, from the moment the patient makes an appointment to the moment the claim is processed and paid to the provider. Everyone in your office plays a key role in the success of the revenue cycle: the receptionist, biller, coder, provider, and practice administrator. It's important to understand how your role affects the revenue cycle.
The order in which you submit your claims can also affect your revenue. Let's look at the following example:
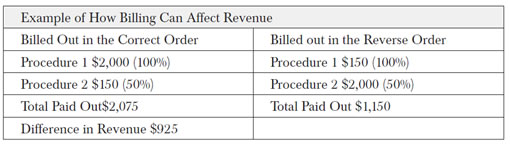
By submitting the procedures in the wrong order as in the example above, the practice could risk losing $925.00.
Another important aspect of the revenue cycle is knowing how to link the diagnosis codes to the proper CPT® codes to meet medical necessity and get the claim paid.
Let's review the flu shot:
- If Medicare (depending on your Medicare Carrier)
Q0236 - Flu Vaccine ( your Q code depends on the ACTUAL vaccine administered to patient)
G0008 - Administration of Flu Vaccine
DX Code: v04.81 - To bill a commercial carrier:
90658 - Flu Vaccine
90471 - Administration of vaccine
DX Code: V04.81 - Changes if it was the FluMist
This is a small sampling as there are multiple vaccine codes for the flu. In the example above, make sure the provider adds the administration. You can't do one procedure without the other. It's important for the billing and coding staff to view the charge ticket for any money that may have been left on the table. In this example the administration can vary from $15 to $30. That's a lot to leave behind so be sure to review the billing before it goes out. To properly bill, your billing and coding staff need to be aware of the companies with which you contract. In the above example, had the biller billed the CPT® codes to Medicare (depending on your Medicare Carrier), the claim would have been denied.
Medical billing should never be viewed simply as data entry. Each claim should be reviewed for accuracy and proper linkage between the diagnosis code and the correct CPT® code. A biller who links all the diagnosis codes to all the procedure codes does not fully understand how the revenue cycle works.
There are times when an Explanation of Benefits (EOB) could be wrong. For example, what if the patient doesn't update the coordination of benefits with the carrier? This could cause an EOB to print incorrectly, thinking the patient has a secondary plan. Such an error will also cause your system to post the payment incorrectly. For these reasons, it's important to review the EOBs for accuracy and to contact the carrier immediately if you find any discrepancies.
Know how to read denial codes such as PR204 (Patient responsibility - other coverage), CO50 (Medical Necessity), and the proper steps to correct denials or rejections. For the Medical Necessity rejection, review the billing. Make sure the diagnosis code was properly linked to the correct CPT® code.
Know the timely guidelines for your carriers as well as the guidelines for submitting a corrected claim. Know if your carrier requests that you use their forms for appeals.
Allow your monthly statements to assist in your collection efforts by using the US Postal Ancillary Services such as the NCOA Link , Return Service, Address service, and Temporary Return services, just to name a few.
Have you ever lent someone money and hated having to ask for repayment? This is the elephant in the room; billers often feel the same way when addressing payment with patients. In such times you need to address the issue with kindness and a professional attitude but remain assertive. Never end a collection conversation without collecting at least a third of what's due with a payment schedule for the balance. Be sure to offer patients different payment methods such as online payments, credit card payments, and checking or savings payment options. The practice should set the tone for payment; you do not have to accept $5 a month simply because the patient said so. Know your rights as they can vary from state to state.
Yvonne D. Dailey, CPC, CPC-I, founded Dailey Billing Services in 2001 to provide electronic medical billing services and she has over 10 years of experience in the medical billing and coding field. She has experience as an adjunct instructor for business schools in her area and is currently a PMCC instructor, providing seminars for physicians, their staff, and new coders.

