There has been a paradigm shift in hospitals today, from a Centralized Scheduling Unit focused on a single task to a fully-integrated Pre-Encounter Department. There are many catalysts for this change, including increases in uninsured or underinsured patients, regulatory changes, and payer requirements. Perhaps yours was one of the facilities leading the industry toward a comprehensive pre-encounter focus. If not, it is time to assess your organization's readiness for this transformational change, and to prepare for the implementation that will bring the facility in-line with this aspect of industry best practices.
This edition of IMA Insights will help you assess your current pre-encounter activities, and will offer suggestions to help transform a mature scheduling practice into a Pre-Encounter Department with a fully-integrated workflow that includes centralized scheduling, pre-registration, financial clearance, payer authorization, and point of service (POS) collection. We will provide an overview of the alignment of resources, technology, and process that is necessary to ensure Best Practice performance.
Background
The days of scheduling a patient and waiting for him or her to present for service before obtaining all the financial, demographic, and medical information, are long gone. With the economic wellbeing of hospitals seemingly under attack from all directions, it is critical that revenue cycle management team members take an aggressive step forward in the integration of the scheduling, pre-registration, insurance verification, pre-certification, registration, and POS collection efforts.
A decentralized scheduling and pre-registration function often leads to missed opportunities in obtaining required authorizations and collection of co-payments, co-insurance, and deductibles at the point of service. Members of the service department clinical team or ancillary clerical staff, whose focus is not on revenue integrity, are at times responsible for scheduling and pre-registration. These personnel are often hampered by time constraints and have other competing priorities. Time constraints and limited focus lead to a negative financial impact that will result in payment delays, denials, rework, and ultimately, financial loss.
The Access Team is the first line of contact with the patient. They should have the responsibility to ensure the integrity of the entire revenue cycle. They must understand the importance of their role in the collection of information and the process of obtaining all the necessary authorizations and financial clearances. Payer demands for preauthorization require scheduling personnel who can interpret physician orders and understand the associated procedure codes. Large patient pay amounts have made financial clearance procedures ever more important, and in the process have changed the responsibilities and corresponding knowledge base of the Access Team. Patient pre-encounter interviews must now be viewed as an opportunity to offer the entire range of account resolution options; hence the need for an integrated pre-encounter approach.
Let's take a moment to gauge your organizations current performance. The following worksheets will help you identify areas of opportunity. Is your team meeting or approaching Best Practice standards, or are there opportunities for improvement?
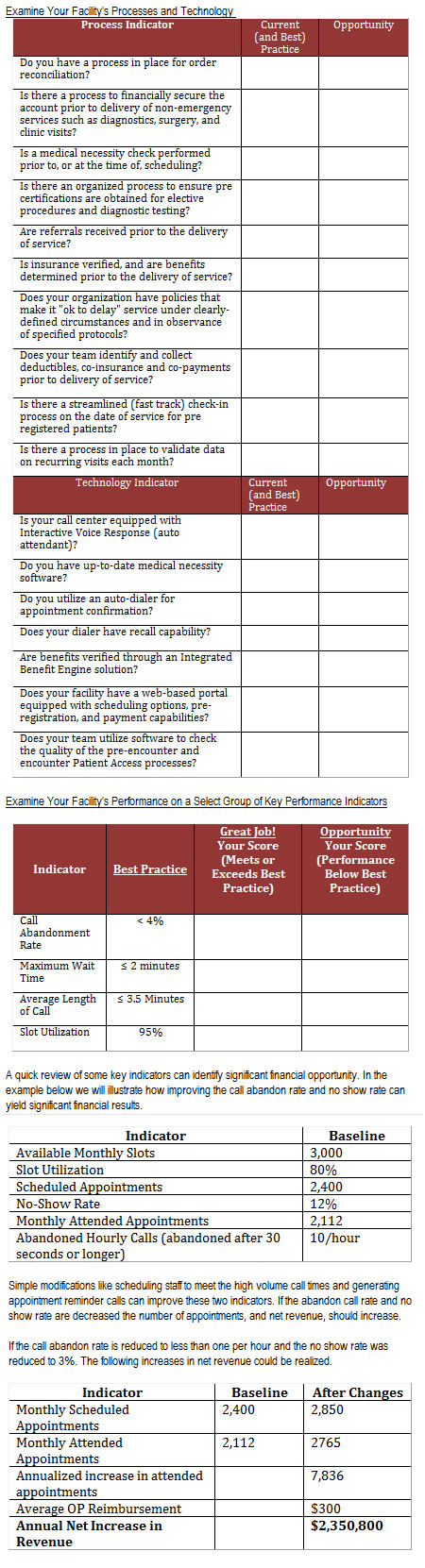
Insights
A fully-integrated Pre-Encounter Department requires highly-skilled staff. A robust training and education program is an essential component. The education program should consist of classroom training, along with role-playing and conversational scripting. Consider online training as part of the overall training initiative. Post-training follow-up should include random quality reviews. Providing staff with a weekly quality report card will enable leadership and staff to acknowledge successes and identify areas of opportunity.
Employee selection is critical to a Pre-Encounter Department's success. Your team should be highly-motivated, energetic, well-organized and good communicators. To meet today's challenges, candidates must be computer-savvy and must learn new tasks and technology quickly. (See October, 2008 IMA Insights: Managing for Optimal Revenue Cycle Performance - Create a Winning Team.)
Implementing a Career Ladder program can be instrumental in eliminating any perception that a Patient Access position is merely a stepping stone to another job. The program should be designed to recognize and reward staff members who demonstrate excellence in their field of expertise, and it should serve as a foundation to develop future departmental leaders. (For more information about career ladders, see the January 2008 edition of IMA Insights: Career Ladders for Patient Access Staff.)
Establishing benchmarks that are aligned with exemplary customer service is essential. Incentive plans tied to these benchmarks can be great motivators.
Adding the right technology to the Pre-Encounter process can enhance revenue cycle results and improve patient satisfaction. This supporting technology includes POS kiosks, integrated insurance verification, patient out-of-pocket estimator, electronic credit card and check processing, and patient portal access for self-scheduling, pre-registration, and patient payment process. Collection of cell phone numbers and email addresses expands communication options, relative to updates and appointment reminders via secured portal, email, or text. (See the October 2009 issue of IMA Insights: Give Patient Access the Necessary Supporting Technology for the Job.)
Indentifying uninsured and underinsured patients prior to the date of service affords the patient the opportunity to be screened for medical assistance and charity care early in the revenue cycle. Using a third party vendor to assist with the financial assistance screening process can result in a positive return on investment for the organization. Serving as an extension of the Pre-Encounter Department, the vendor can provide the subject matter expertise that is necessary to qualify patients for Medicaid, Disability and Charity. By proactively indentifying patients that need financial assistance, a facility can decrease bad debt and improve patient satisfaction.
Summary
For several years, Revenue Cycle focus has been shifting to front-end processes. The Pre-Encounter Department is a logical culmination of that focus; and is one way to ensure optimal financial and customer satisfaction results, through the integration of centralized scheduling, pre-registration, financial clearance, payer authorization, and POS collection. Staffing that department with talented people who are well-trained and motivated, in addition to implementation of efficient processes and supporting technology solutions, will help to provide your patients with a positive service experience while improving the hospital's financial position.
We are pleased to have the opportunity to present this information to you. If you have any questions or need assistance in enhancing your pre-encounter processes or organizational structure, please contact Kim Hollingsworth, Partner, at (610) 517-1386.
Best Regards,
Terri Donohue
Senior Consulting Manager
Betsy Keating
Consulting Manager
Linda Koontz
Consulting Manager
Helene Montini
Senior Consulting Manager
